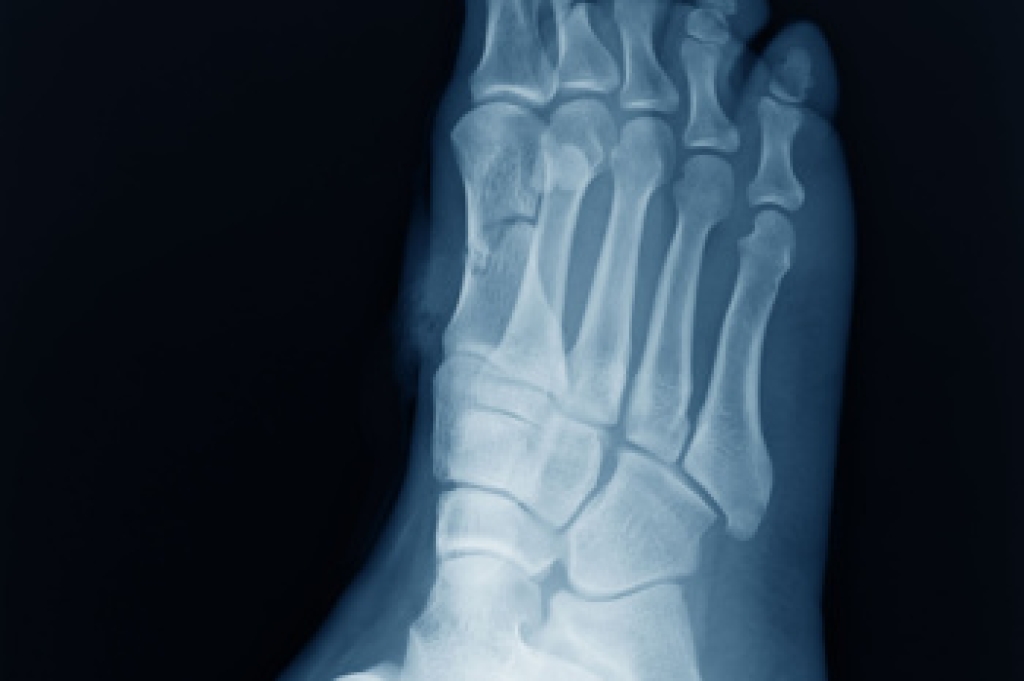
Broken toes or feet often result from trauma, such as stubbing the toe, dropping a heavy object on it, or from sports injuries. Immediate first aid is important in managing pain and preventing further damage. First, immobilize the injured area to prevent movement. Use a splint or tape the broken toe to an adjacent toe for support. Elevate the foot above heart level to reduce swelling. Avoid putting weight on the affected foot to prevent further injury. Pain relievers can help to manage pain and inflammation. Seek medical attention from a chiropodist as soon as possible. If you believe you have broken a toe or foot, it is suggested that you visit a chiropodist who can provide a proper diagnosis through physical examination and imaging, like X-rays. They will recommend an appropriate treatment plan, which may include casting, protective footwear, or in severe cases, surgery.
Broken toes or feet often result from trauma, such as stubbing the toe, dropping a heavy object on it, or from sports injuries. Immediate first aid is important in managing pain and preventing further damage. First, immobilize the injured area to prevent movement. Use a splint or tape the broken toe to an adjacent toe for support. Elevate the foot above heart level to reduce swelling. Avoid putting weight on the affected foot to prevent further injury. Pain relievers can help to manage pain and inflammation. Seek medical attention from a chiropodist as soon as possible. If you believe you have broken a toe or foot, it is suggested that you visit a chiropodist who can provide a proper diagnosis through physical examination and imaging, like X-rays. They will recommend an appropriate treatment plan, which may include casting, protective footwear, or in severe cases, surgery.
A foot fracture is a crack or break in a foot bone, often caused by repetitive stress on the foot or a high-impact foot injury. If you’re suffering from foot pain, please consult with one of the specialists from Thornhill Foot Clinic. Our chiropodists can help you maintain the health of your lower limbs and your mobility.
Symptoms
- Pain
- Bruising
- Tenderness
- Swelling
- Difficulty walking
- Deformity
Causes
- Repetitive overloading of the foot
- Having a previous fracture
- Abnormal foot biomechanics
- Changing training surfaces suddenly
- Poor footwear
- Osteoporosis
- High-impact injury
Treatments
- Rest
- Ice
- Elevation
- Pain medication
- Braces or other orthotics
- Casts
- Crutches
- Surgery in more severe cases
If you have any questions, please feel free to contact our office located in . We offer the newest diagnostic and treatment technologies for all your foot care needs.