The tarsal tunnel is a narrow space on the inside of the ankle, located next to the ankle bones. Within the tarsal tunnel are a variety of tendons, arteries, veins, and nerves, including the posterior tibial nerve. Tarsal tunnel syndrome is a condition that occurs when the posterior tibial nerve is squeezed or compressed. This can happen due to injuries that produce inflammation or swelling near the nerve, systemic diseases like arthritis, an abnormal structure such as a cyst putting pressure on the nerve, or flat feet straining the nerve as you walk.
Symptoms of tarsal tunnel syndrome include tingling, burning, or electrical shock sensations in the inside of the ankle or bottom of the foot, as well as numbness and shooting pains. In some cases, the symptoms are isolated to one small area, like the inner ankle. In other cases, the symptoms may affect the entire foot and ankle. Symptoms typically occur during or are aggravated by physical activities like walking, running, jumping, or prolonged standing.
Tarsal tunnel syndrome can be diagnosed by a chiropodist through physical examination of the affected foot and ankle. Imaging studies may be used if the chiropodist suspects that the underlying cause may be a structural abnormality, like a cyst. Treatment options for this condition include resting and icing the affected area, taking oral medications to reduce pain, immobilizing or bracing the affected foot, wearing supportive shoes or orthotic inserts, and physical therapy. Left untreated, tarsal tunnel syndrome can lead to permanent nerve damage.
If you are experiencing the symptoms of tarsal tunnel syndrome, please consult with a chiropodist.
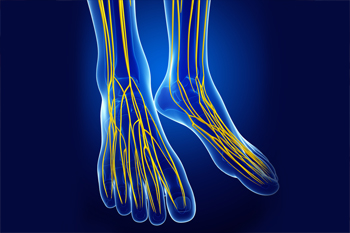
Tarsal tunnel syndrome is a nerve disorder. Those with this condition often experience pain in the ankle, foot, and toes. Tarsal tunnel syndrome is caused by the compression of the posterior tibial nerve, which runs through a canal near the heel and into the sole of the foot. When the tissues around this nerve become inflamed, they can press on the nerve, therefore, causing pain. If you have symptoms of this syndrome, contact a chiropodist who is dedicated to foot health and can offer you the best treatment plan.
Tarsal tunnel syndrome can cause pain and progress over time. If you are experiencing any symptoms of tarsal tunnel syndrome, please consult with one of the specialists from Thornhill Foot Clinic. Our chiropodists will assess your condition and provide you with quality foot and ankle treatment.
What Is Tarsal Tunnel Syndrome?
Tarsal tunnel syndrome is a condition in which the posterior tibial nerve, which is located within a structure called the tarsal tunnel on the inside of the ankle, is squeezed. Compression of the posterior tibial nerve can be caused by injuries, such as ankle sprains, systemic diseases like diabetes or arthritis, strain on the tarsal tunnel due to flat feet, or an enlarged structure like a cyst squeezing the nerve.
Symptoms
Symptoms of tarsal tunnel syndrome can appear suddenly and are generally worsened by physical activity.
Common symptoms include:
Tingling, burning, or electrical shock sensation on the inside of the ankle or bottom of the foot
Numbness
Shooting pain
Diagnosis
Tarsal tunnel syndrome is diagnosed through physical examination. If initial treatment is ineffective, imaging or nerve studies may also be necessary.
Treatment
Nonsurgical treatments for tarsal tunnel syndrome include resting and icing the foot, bracing or immobilizing the foot, wearing an orthotic device, modifying your footwear, and taking medications to relieve pain. Surgery may be needed if nonsurgical treatments are ineffective.
If you have any questions, please feel free to contact our office located in . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Though diabetes begins with the pancreas not producing enough insulin, thus raising your blood sugar levels, it is a systemic condition that can affect every part of your body. The feet are no exception, and a variety of lower limb problems are very common among people with diabetes.
One of the primary foot-related concerns for patients with diabetes is diabetic foot ulcers (DFUs). These are poorly healing open wounds on the feet that are at high risk of becoming infected due to a weakened immune system, another common complication of diabetes. Nerve damage in the feet caused by high blood sugar levels interferes with pain signaling between the peripheral nerves in the feet and the central nervous system (the brain and spinal cord). When this signaling is disrupted, it can be difficult to detect foot injuries, such as cuts and scrapes, when they occur. These injuries are then left unnoticed and untreated until they have significantly worsened. Poor circulation, another complication of diabetes, means that not enough nutrients reach the feet. Without them, the wounds on the feet heal slowly and poorly, or not at all. These wounds can then become infected, leading to tissue death.
The best way to prevent DFUs and their consequences is to carefully monitor the health of your feet through daily foot inspections. Using a mirror to help you see your feet fully, look for any cuts, scrapes, sores, bruising, swelling, discoloration, rashes, hair loss, deformities, or nail changes. Take note of any foul odors, pain, warmth, and strange sensations such as numbness, tingling, burning, or pins and needles. If you notice a problem, seek the care of a chiropodist as soon as possible. Early treatment is key to avoiding potential complications.
DFUs are not the only foot problem diabetics are more likely to encounter. Diabetes can also increase your risk of corns and calluses, cracked skin, bunions, hammertoes, Charcot foot, nail disorders, and various infections. If you have diabetes, it is strongly suggested that you are under the care of a doctor who can help you monitor your foot health, treat any existing conditions, and prevent future ones.
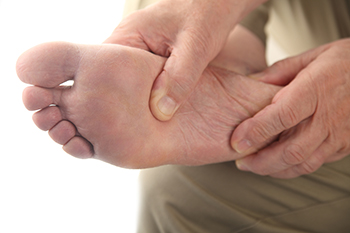
Diabetic patients can encounter foot problems if basic care needs are not met. Diabetes can occur as a result of elevated blood sugar levels and can come from specific foods that are eaten. Neuropathy is a common condition that can happen from being diabetic, and this is the inability to feel existing cuts and scrapes on the feet. The feet can become numb, and untreated injuries may develop into serious foot issues. Diabetic foot care can begin with checking the feet every day, and this can be done by using a mirror if a family member or caregiver is not present. This can be preceded by washing and drying the feet thoroughly and trimming the nails weekly. Many people choose to visit a chiropodist to have this done, which may help to eliminate ingrown toenails from developing. It is beneficial to monitor glucose levels daily, and this can help to educate the patient about which foods produce high sugar levels. People who smoke may have poor circulation, and it is suggested that smoking is stopped to ensure proper blood flow. Maintaining good foot care is crucial in diabetic patients, and it is strongly suggested that you are under the care of a chiropodist who can help you to manage this condition.
Diabetes can cause serious problems in the lower limbs if proper preventive measures are not taken and diabetic wound care is not performed. If you would like to learn more about caring for diabetic feet, please consult with one of the specialists from Thornhill Foot Clinic. Our chiropodists can help you maintain the health of your lower limbs and your mobility.
Diabetes can lead to a host of foot and ankle complications, including:
Poor circulation
Peripheral neuropathy
Diabetic foot wounds and ulcers
Infection
Corns and calluses
Dry, cracked skin
Nail disorders
Hammertoes
Bunions
Charcot foot
If you have diabetes, you must be vigilant of any changes in your foot health. This is best done through daily foot inspections. Using a mirror to help you if necessary, look for any:
Cuts, scrapes, sores, or wounds
Bruising or discoloration
Swelling
Rash
Foul odor
Nail changes
Hair loss
Warmth and inflammation
Deformities
Lower limb pain
Strange sensations (numbness, tingling, burning, pins, and needles)
If you detect anything unusual, seek the care of a chiropodist as soon as possible. If you have any questions, please feel free to contact our office located in . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ankle fractures occur when one or more of the bones that make up the ankle are broken. This typically occurs following a sudden injury, such as stepping off a curb and severely twisting your ankle or suffering a strong impact while playing a sport.
Symptoms of an ankle fracture can include pain at the site of the break, swelling, bruising, blistering, difficulty walking and bearing weight on the affected ankle, and ankle deformity. In the case of an open fracture, the broken bone pokes through the skin, increasing the likelihood of infection and further complications.
Ankle fractures require prompt medical treatment. They can be diagnosed through physical examination and imaging studies, such as X-rays or bone scans. Treatment varies depending on the severity of the injury and may include resting, icing, compressing, and elevating the affected ankle, immobilization of the ankle, and taking pain medications. Surgery may be necessary in more severe cases. If you have injured your ankle, please seek the care of a chiropodist.
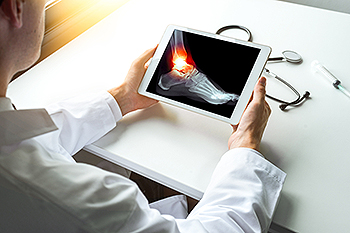
There are different types of ankle fractures, consisting of partial and complete. A partial break refers to a bone that is slightly cracked, as its name implies. A thorough fracture is a complete break, and the bone ends up in two pieces. Many broken ankles are treated by wearing a cast or a protective boot, and this is often adequate in providing the necessary support as the healing process occurs. For severe fractures, surgery may be required to ensure complete healing. This is advised if the bones are displaced, or tendons and ligaments are torn. There may be metal pins, screws, or plates inserted in the foot that hold the bones in place as the ankle heals, and possibly removed at a later date if necessary. Patients have found mild relief when the affected foot is frequently elevated, and mild pain relievers may be suggested for pain and discomfort. If you have fractured your ankle, please schedule an appointment with a chiropodist sooner rather than later who can recommend the treatment option that is correct for you.
test template
Plantar hyperhidrosis is a medical condition that causes the feet to sweat excessively. It typically affects both feet equally. Plantar hyperhidrosis can greatly affect one’s life. When the feet sweat too much, they can become chronically damp, cold, white, and pruney. The skin of the feet becomes a perfect breeding ground for a variety of fungi and bacteria that thrive in moist environments. Infections like athlete’s foot can spread on the feet and to the toes and other parts of the body. The feet may also produce a strong, unpleasant odor.
Plantar hyperhidrosis can also affect your footwear. Excessive sweat can ruin your shoes over time. The moisture may also cause your feet to slip around or out of the shoes, becoming a serious safety hazard. Friction blisters also become more likely. At the same time, you may not want to take off your shoes, in fear of leaving behind damp footprints or having someone notice the state of your feet.
Fortunately, a variety of treatments are available to reduce sweating and improve your quality of life. The first line of treatment is usually a topical antiperspirant. These can be bought over the counter at the drugstore or prescribed by your chiropodist. They typically come in the form of a gel, powder, or cream and are applied directly to the feet to prevent sweat from reaching the surface, much like the antiperspirants you might find in your deodorant. Another option is taking oral medications to temporarily reduce excessive sweating. Iontophoresis, a treatment that uses electrical currents conducted through water to reduce hyperactivity in the sweat glands may help. In some cases, more invasive treatments, like botox injections directly into the feet to disable the sweat glands, may be prescribed.
To learn more about plantar hyperhidrosis and to find the right treatment for you, please consult with a chiropodist.

A condition known as plantar hyperhidrosis, or more commonly sweaty feet, can be annoying and even embarrassing. Some people sweat so much that their feet slide around in their shoes. Sometimes the feet can become infected and smell bad. Hyperhidrosis also can cause the feet to feel cold because they are continuously wet. While the cause of plantar hyperhidrosis is not clear, it seems to be a case of overactive sweat glands that are inherited. Sweaty feet are more common in men than in women and more common among young adults. It is wise to wash your feet daily with antibacterial soap to ward off infections that may cause foot odor. Using an antifungal foot powder may also help. Absorbent shoe inserts and moisture-wicking socks are suggested. Drying out your shoes thoroughly after wearing them and alternating shoes each day are good ideas. A chiropodist can offer a number of other treatment options, including Botox injections and certain prescription medications. For more information, please consult a chiropodist.
Plantar hyperhidrosis is a medical condition that causes excessive sweating of the feet. This problem is not only embarrassing but can also cause a variety of foot health problems if left untreated. Fortunately, there are many effective treatments available for plantar hyperhidrosis. If you have very sweaty feet, please consult with one of the specialists from Thornhill Foot Clinic. Our chiropodists can help you maintain the health of your lower limbs and your mobility.
Signs & Symptoms
Excessive foot sweat
Sweating from both feet
Slipping out of shoes due to sweat
Damp footprints
Ruined shoes
Frequent foot infections
Friction blisters
Whitish foot color
Wrinkly, pruney feet
Cold feet
Strong odor
Treatment Options
Topical antiperspirants - Powders, creams, or gels that are applied directly to the feet to prevent sweating; can be over the counter or prescription strength
Oral medications - Pills taken by mouth to reduce sweating temporarily
Iontophoresis - A procedure that uses a mild electrical current conducted through water to reduce activity in hyperactive sweat glands
Botox - Injected into the feet to prevent activation of sweat glands
In addition to these treatment options, footwear modifications, such as wearing shoes and socks made of breathable or moisture-wicking materials, are also suggested. If you have any questions, please feel free to contact our office located in . We offer the newest diagnostic and treatment technologies for all your foot care needs.