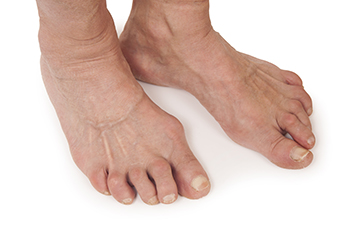
Osteoarthritis is a condition in which the cartilage located on the ends of joints deteriorates over time. Cartilage is very important, as it protects and cushions the bones during movement. Osteoarthritis is the most common type of arthritis and is associated with aging. It can affect any of the joints in the body, and frequently affects the joints of the feet and the ankles. Though rarer, osteoarthritis can also occur as a consequence of an injury, such as as a sprain or fracture, or as a result of abnormal foot biomechanics.
Symptoms of osteoarthritis include pain and stiffness in the joints, swelling, and difficulty walking or bending the joints. In some cases, bony protrusions called bone spurs can develop on the affected joints. Osteoarthritis is a progressive condition, meaning that it worsens over time. Diagnosing the condition early allows for earlier treatment, which can help preserve the health and function of your joints.
A variety of treatment options are available for osteoarthritis. Pain can often be minimized by taking nonsteroidal anti-inflammatory medications, getting steroid injections into the affected joints, and wearing orthotics. Bracing or immobilizing the affected foot or ankle may help reduce inflammation and prevent deformity of the joint. Doing specific exercises can help strengthen the muscles in the feet and ankles to prevent injuries. In cases where more conservative treatments have failed or in which arthritis has progressed significantly, surgery may be an option. If you have osteoarthritis in your feet or ankles, it is recommended that you consult with a chiropodist.